Recruitment Event
BOOK AN APPOINTMENT
CALL 0208 991 5280
More Motion. More Health. More Life.

Welcome to Health in Motion. We invite you to become
the navigator of your body's voyage towards more movement and more health.
BOOK AN APPOINTMENT
CALL 0208 991 5280
Life is too short to endure persistent pain and restriction
Quick fixes only lead to more frustration. You want more than temporary relief; you want to understand your condition and prevent it. If you're unsure where to find a solution, we offer precise knowledge and tools to help you regain comfort.




Our clinic values connecting with patients and the community. Health in Motion goes beyond typical healthcare, listening to your story to find the best solutions for your challenges. Say goodbye to pain and limits, and welcome a life guided by motion for better health. We're more than osteopaths; we're your partners in pursuing a joyful, active life.
"I founded this practice to provide a service that I would value, ensuring that you receive the same level of care I demand for myself." - Lola Phillips
Pain can be scary when its cause is unknown. We're here to help you understand and overcome it, providing relief and prevention strategies.
We're a team focused on your wellness, led by Lola Phillips. With our C.A.R.E Plan©, we ensure a thorough diagnosis and personalised treatment to restore your health.
We understand everyone is unique, so we customise our approach to fit your needs. Whether you need pain relief, injury recovery, or peak performance, we're here to support you throughout your journey.
We hope you will choose Health in Motion Osteopaths as your partner in physical health. Your trust fuels our commitment to excellence as we embark on the voyage of improved health together.
BOOK AN APPOINTMENT
CALL 0208 991 5280
Embark on Your C.A.R.E. Voyage:
Calm, Adjust, Reinforce, Elevate
Our team of expert osteopaths does more than treat symptoms.
We guide you through a transformative journey, reigniting the joy of unrestricted motion.
Our signature C.A.R.E. voyage includes:
Calming your nervous system
Adjusting target areas of your body
Reinforcing your progress
Elevating your health





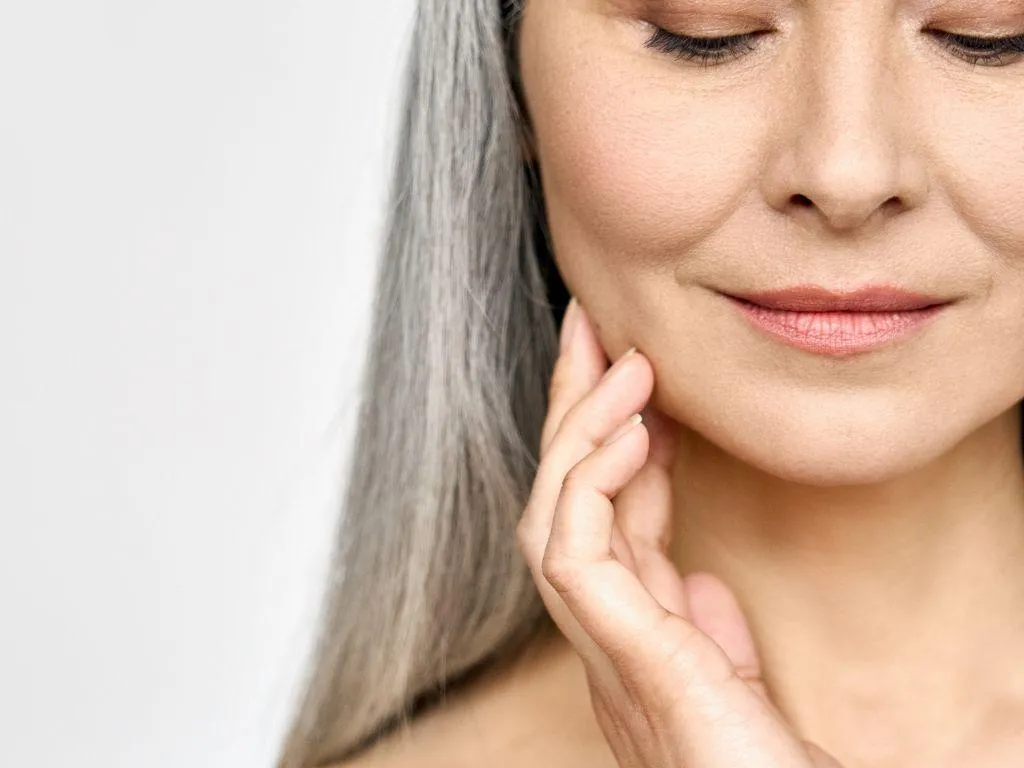
How we work
Initial Consultation


Book your initial consultation by phone or online.
You will be examined by an expert in physical medicine - a Registered Osteopath or equivalent professional.
Follow up Appointments
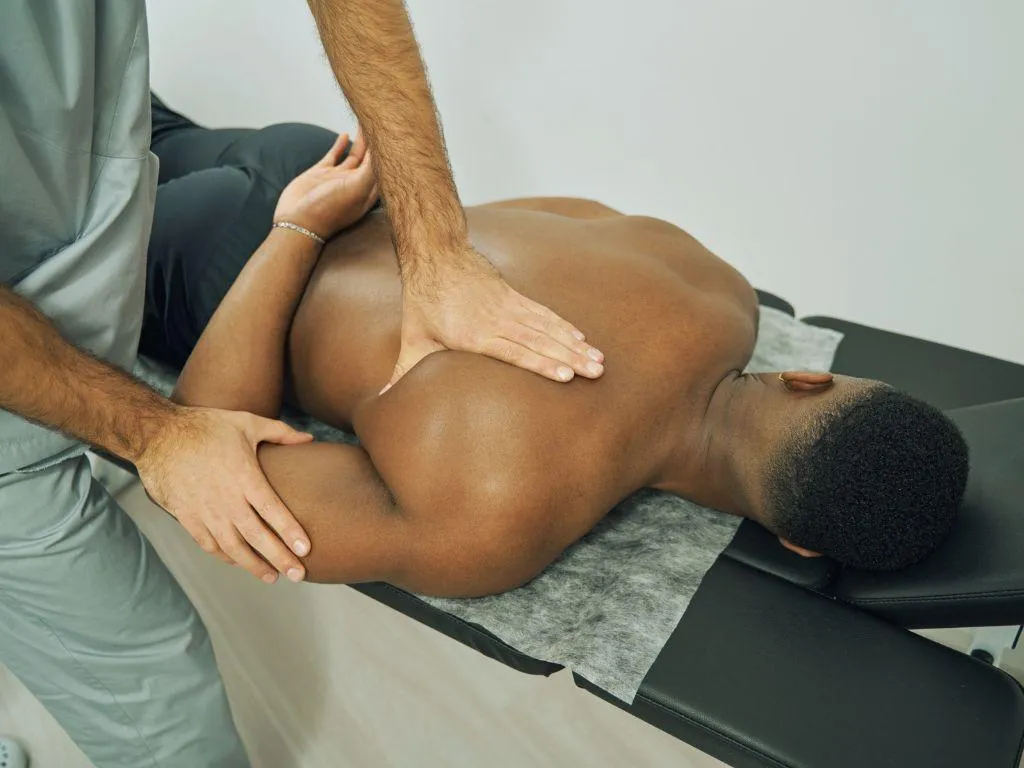

A C.A.R.E report will be emailed to you before your first follow up appointment, outlining our findings, your expected outcomes, and the number of treatments we are prescribing.
When you decide to go ahead with our C.A.R.E plan your adjustment appointments will be reserved at a time that is most convenient for you to attend.
Reclaim your Life


We will provide bespoke advice and movement prescriptions during your C.A.R.E voyage. When we get you to peak physical health, we will discuss your ongoing self care plan.
BOOK AN APPOINTMENT
CALL 0208 991 5280
Start improving your mobility now!
If you are not in pain but would like to improve your mobility then download one of our guides for the Neck, Upper Back, Lower back, Pelvis, Hips, Shoulders, Ankles, and more.